Online CPR Certification Blog
How does stress influence cardiac health and how one lives?
Date: March 9th, 2024
The experience of stress is common and inevitable and can affect your general health. Unhealthy physical conditions, including a lack of sleep or an illness, can also contribute to stress. The emotional toll of things like financial insecurity or the loss of a cherished one is not to be discounted as a source of stress in and of itself.
The stress response in your body is there to keep you safe. However, it might be harmful if it persists over time, releasing the hormone cortisol when under pressure. Scientific evidence suggests chronic stress raises triglycerides, blood cholesterol, and blood pressure. These are typical causes of cardiovascular disease.
Additionally, chronic stress can modify blood clotting. More clots form in the circulation, which raises the possibility of a stroke. Therefore, your ability to cope with stress depends on your ability to identify and address the underlying reasons. Fortunately, this article covers the relationship between stress and heart health and how you may overcome the various types of stress.
Stress and heart health: Understanding stress and its impacts
Stress is the body’s physiological reaction to any situation that the mind interprets as hazardous. Any situation in which you find yourself needing to make adjustments is stressful.
Although stress has a poor reputation, it is not always harmful. There is such a thing as beneficial stress; it’s called eustress.
Stress exists in two categories: Acute and chronic. Both have the potential to influence the body and bring about distinct alterations.
Acute stress
Acute stress disorder (ASD), also known as an acute stress reaction, is a mental health condition that can manifest in those who have experienced or seen a terrible event that threatens their survival.
Simply put, ASD is a psychological disorder that might manifest in the first weeks or months following a traumatic experience.
Some of the traumatic events may include:
- Sexual assault
- Car accidents
- The sudden death of a relative or loved ones
- Finding out you have a terminal illness.
The rapid onset of symptoms following exposure to painful stimuli characterizes acute stress disorder. Individuals with ASD are more likely to suffer emotional and physical signs in response to trauma, including intense feelings of fear and helplessness.
Some of the physical symptoms may include:
- Difficulty breathing
- Pounding heart or palpitations
- Chest pain
- Stomach and headache
- Nausea and sweating
These signs and symptoms usually appear immediately after the traumatic occurrence and may subside within a few days or sometimes just hours. Still, there are occasions where signs and symptoms linger for weeks.
The following psychological effects may also occur:
- Avoidance: Victims always resolve to stay away from anything that might bring back traumatic thoughts, feelings, or physical sensations
- Signs of arousal include heightened awareness, distraction, trouble sleeping, a bad attitude, and explosive rage.
- Dissociation: Physical disorientation, such as perceiving oneself from outside the body, feeling dizzy, having one’s sense of time altered, or having trouble recalling the event.
- Depression The inability to experience and show happiness consistently
- Intrusion: Repetitive, uncontrollable memories of the trauma, including nightmares
Chronic stress
Acute stress, a severe physical and mental response to a sudden and unexpected occurrence is something that many people may encounter at some point in their life. However, chronic stress is characterized by ongoing but manageable tension and anxiety.
Therefore, chronic stress, long-lasting or prolonged stress that can impact both your psychological and physical well-being,
Constant stress responses can disrupt work, relationships, and health. A common symptom of persistent stress is a sense of being “stuck.
Your respiration and heart rate will stay elevated, your muscles will remain tense, and your digestion may become impaired as you deal with this form of stress. You might also find that your immune system is weaker.
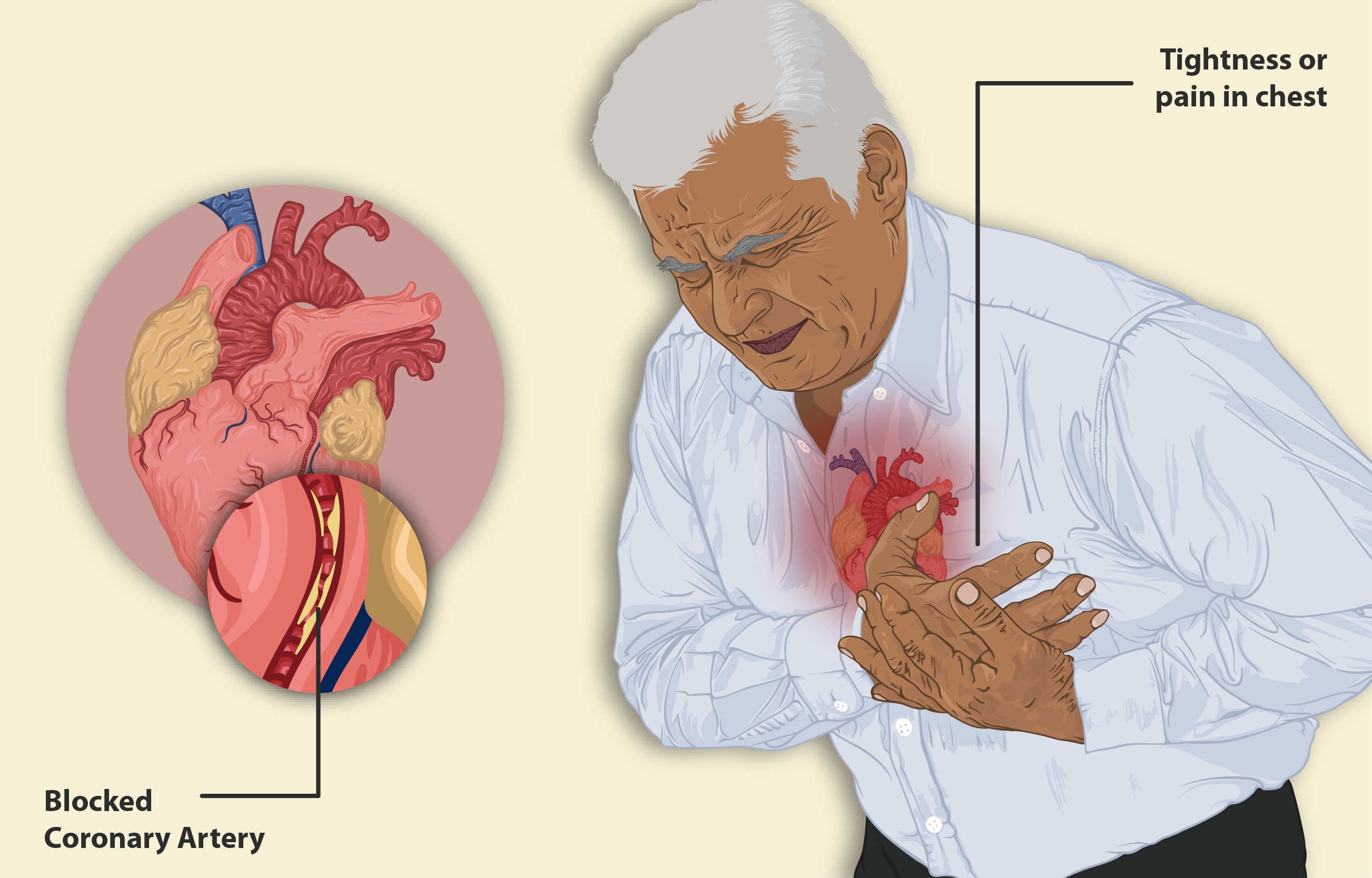
Image alt text: stress and heart health. An image of a person suffering from chest tightness as a result of cardiac arrest.
Author credit: By https://www.myupchar.com/en – https://www.myupchar.com/en/disease/angina, CC BY-SA 4.0, https://commons.wikimedia.org/w/index.php?curid=81374128
Chronic stress can have a variety of reasons.
- High-stakes work
- Money or financial problems.
- Tense interactions or relationships
- The practice of bias or racism
- Dealing or coping with a long-term health condition
The effects of chronic stress on the body are cumulative and long-lasting. This can bring on a wide variety of symptoms and increase the likelihood of getting sick.
Here are some of the chronic stress symptoms to watch out for:
- Emotional withdrawal
- Weak in spirit/low energy
- Thinking that is scattered or muddled
- Appetite Alteration
- Helplessness or struggle to cope
- Low or negative self-perception
- Sleeplessness or insomnia
- Extreme irritability, discomfort, and pain
- Abuse of drugs and alcohol increases
- Altering one’s emotional reactions to other people
- Nervousness
- Lack of sexual desires
- sickness or infection that occurs frequently
The effects of stress on the human body?
It’s been found that people’s reactions to stressful events vary greatly. Some people have pretty powerful responses. Some people are easygoing and carefree. The stress response occurs when the body adjusts to face adversity. As soon as you register a stressful or frightening stimulus, your brain initiates the stress reaction.
The body’s reaction to stress consists of two main parts:
Cortisol
The “stress hormone,” cortisol, is produced more significantly by the brain in response to exposure to a stressful situation. To help you cope with stressful situations, cortisol boosts your energy levels. It accomplishes this by facilitating the release of glucose from the liver into the bloodstream, which can be used for energy production.
Epinephrine and norepinephrine
A different region of your brain sends messages to your adrenal glands to produce more of the stress chemicals adrenaline and norepinephrine. Many people use the term “fight or flight” to describe this aspect of their body’s stress response. A rise in these hormones helps your body get ready to deal with stress by doing the following:
- Reducing digestion
- Increasing your energy reserves
- Inducing a rise in blood pressure and heart rate
- Increasing the frequency of your breaths
- Improving muscular oxygenation and circulation
Stress and heart health: How does stress affects your cardiac health?
Researchers in 21 nations analyzed data from 118,706 individuals in 2021 who had no preexisting cardiac disease. In general, the researchers observed that high-stress levels were connected with a greater risk of:
- High blood pressure
- Stroke and heart attack
- Diabetes
- Unhealthy lifestyle behaviors
- Death
Chronic stress may cause:
Inflammation of the cardiovascular system
The American Heart Association suggests precise data proving a link between cardiovascular disease, physiological health, and risks.
Also, according to studies, the amygdala (a region of the brain responsible for emotional processing) sends a command to the red marrow to increase the production of white blood cells when the body is under stress. High levels of stress hormones in the bloodstream are associated with elevated glucose levels in the blood.
When blood sugar levels rise over what the body needs, inflammation develops along the arterial walls, and a heart attack or stroke may result from developing cholesterol-rich plaque in the arteries due to this inflammation.
Stress Cardiomyopathy
Stress cardiomyopathy, also known as takotsubo cardiomyopathy, is a condition in which the heart muscle weakens due to prolonged exposure to high levels of mental or physical stress.
The rapid onset of disease, the experience of severe trauma, witnessing a natural disaster, the death of a loved one, or the overwhelming presence of a dreadful fear can all serve as triggers. Broken heart syndrome is an alternative term for the illness.
This condition is often characterized by the sudden development of angina-like chest discomfort, shortness of breath, and other heart attack-like symptoms. While the remainder of the heart continues to pump with the same or increased force, the left ventricle swells and becomes less efficient.
Fortunately, most episodes are short-lived, and once treated, patients can anticipate a full recovery of cardiac function within a few weeks. Sometimes it can be fatal, but only rarely. Because of this illness, people have realized how dangerous stress can be to the heart and blood vessels.
Leads to unhealthy lifestyle behaviors
Regular exercise, a healthy body weight, and a nutritious diet are all things we’ve been told will help keep our hearts healthy and help us live healthy lives. However, you might not know that stress can increase the likelihood of engaging in unhealthy behaviors or activities that are bad for your heart.
Indeed, physical, mental, and behavioral changes can result from stress. Recognizing the signs of stress early will help you deal with it. But how can stress affect your health?
First, let’s consider some of the healthy behaviors you need to lead a good heart life. You must:
- Control your stress level
- Manage or moderate your alcohol consumption
- Eat well and get regular exercises
- Quit or stay away from nicotine products
- Manage your weight
Unfortunately, there’s a correlation between stress and lifestyle behavior change, and experiencing chronic stress has the potential to increase your risk of heart complications through:
- Higher alcohol consumption
Alcohol disrupts the delicate physiological balance maintained by the hypothalamic-pituitary-adrenal or the (HPA) axis system and increases the risk of injury to the body.
Increased cortisol production from alcohol consumption changes the brain’s chemical makeup and restores physiological norms. A change in the body’s hormone levels caused by alcohol consumption alters how stress is experienced and dealt with. Even worst, cortisol has been shown to facilitate the formation of new habits, which can double the likelihood that a person will develop an alcohol addiction.

Image alt text: stress and heart health. A pictorial illustration of a human heart.
Author credit: By Zythème – Own work, CC BY 4.0, https://commons.wikimedia.org/w/index.php?curid=109957995
So, how do stress and alcohol affect your heart?
Drinking an unhealthy amount of alcohol can increase the risk of developing elevated blood pressure, heart failure, and stroke. Consuming excessive alcohol can also have a role in the development of cardiomyopathy, affecting the heart muscle.
In addition, drinking alcohol can be a factor in the development of obesity, which is associated with a lengthy list of potential health concerns.
- Stress and weight
Scientists have known for a long time that increased levels of cortisol are associated with a greater likelihood of putting on weight. When you’re feeling anxious, your body releases the hormones adrenaline and cortisol, which cause glucose to flood your blood. Everything is done to ensure you have the strength to flee a potentially dangerous scenario.
When danger is no longer present, the body’s natural response of releasing adrenaline and lowering blood sugar levels begins. Now is when your body’s production of cortisol goes into overdrive to restore your energy levels.
The hormonal shifts that accompany stress aren’t the only thing that can lead to weight gain; stress can also motivate the following bad habits:
Emotional/affective eating: Not only can elevated cortisol levels increase your desire for unhealthy fare, but anxious energy can lead to uncharacteristically excessive snacking.
It’s possible that eating more food than you need to relieve stress in the short term could make it more challenging to maintain a healthy weight in the long run.
Reduced sleep time: Many people have problems drifting off to sleep when under pressure. And there’s evidence that not getting enough sleep can impede your metabolism. Oversleeping can lead to a loss of self-control, which increases the likelihood that you’ll indulge in unhealthy snacking, thus increasing your weight.
Stress also increases heart-related risk factors, including:
High blood pressure
High blood pressure occurs when blood pushes too hard against the arterial walls.
Stress causes an increase in hormone production in the body. Short-term elevation of blood pressure due to these hormones’ instigation of increased heart rate and constriction of blood vessels. And when blood is forced through constricted walls, the result is increased blood pressure which is a risk factor for heart complications.
High blood pressure, coronary disease, and stroke are all conditions that inappropriate responses to stress may exacerbate. There is also a correlation between some actions and hypertension.
- Smoking
- Abusing alcoholic beverages
- Intake of unhealthful foods
High risk of diabetes
While it’s true that stress isn’t the direct cause of diabetes, it can certainly complicate the illness and make it harder to manage.
Having to deal with diabetes on top of life’s other ups and downs is stressful. Living with it isn’t always simple, and it can feel even more so when many other people don’t understand your situation.
So, how exactly does stress increase your risk of diabetes?
When experiencing stress, your body secretes cortisol and adrenaline hormones to offer you more stamina for the “fight or flight” reaction. However, the hormones play a role in insulin resistance, a condition that reduces insulin’s efficacy. High blood sugar occurs when your body’s cells are unable to absorb the energy you consume.
Simply put, persistent stress raises the risk of hyperglycemia and its attendant consequences, such as cardiovascular disease and cerebrovascular accidents. As a result, it can harm your mental and emotional well-being, as well as your ability to take care of yourself.
How to Reduce Stress for Heart Health
Luckily, you can lessen the impact of stress on your health. Recognizing what is causing you stress is the first step. Despite how challenging it may be, make an effort to manage your emotional and physical responses to these trying circumstances. Try these techniques to reduce stress and maintain cardiovascular health.
Establish a solid foundation of support
The stress you feel and the likelihood of developing heart disease may be lowered if you have a solid supporting group, such as a spouse, a close friend, a religious community, or some other group you regularly join.
Even if you already suffer from heart disease, joining our network can lessen your chances of having another attack. When you have someone you can count on, you feel less alone and more supported.
Having a solid group of people in your corner encourages you to prioritize your own health and wellness. Besides, studies link a lack of appropriate social or interpersonal to various adverse health behaviors, including smoking, poor diet selection, and excessive alcohol consumption.
Lower your stress level at work
Stress from a demanding profession with limited options for personal growth or payoff has been linked to an increased risk of heart disease. Workplace stress will be even more of an issue if you suffer from chronic anxiety or lack a solid support system.
Take charge of your situation if you can’t locate a different job within your organization. Make an effort to take a break from work every day. Get some rest by engaging in a pastime you appreciate. The activity could be as simple as reading, walking, or even taking deep breaths.
If you’re having trouble dealing with stress and anxiety, see if your company provides an employee assistance program (EAP). A therapist might suggest techniques to help you cope with stress at work.
Do a lot of physical activity
The negative effects of stress can be mitigated through physical activity. Heart health experts recommend up to 150 minutes of vigorous exercise weekly. How, then, does physical activity boost cardiovascular fitness?
By assisting with weight management, enhancing cholesterol levels, and decreasing blood pressure, exercise is a great way to boost or lessen your chances of cardiovascular complications.
In addition to helping you feel better overall, exercise can also make you feel less stressed—those who regularly exercise experience less of a physiological reaction to stress. As a result, they don’t experience the same heart rate or blood pressure increases as non-exercising stressed individuals.
Bladder problems and depressive disorders are additional risk factors for cardiovascular disease, but regular exercise can help mitigate this threat.
Seek help if you’re struggling with persistent depression or worry/anxiety
If you currently have heart disease, despair and anxiety can worsen your condition and raise your risk of dying.
Evidence suggests that persistent emotional or mental stress raises the probability of a cardiac arrest-related fatality. Yoga, walking, conventional meditation, guided imagery, and other stress-reduction techniques can all help lower anxiety. Find local training opportunities.
Anxiety, stress, and hypertension can all be exacerbated by consuming alcohol, tobacco, or caffeine. There is some evidence that reducing or eliminating these substances can help relieve stress, depression, and anxiety. If you are feeling depressed or anxious, discuss your feelings with your doctor and ask about possible medications that could help.
Conclusion
Stress and heart health are somehow linked and experiencing high stress level is dangerous for your hear. Consult your doctor if you feel that your stress levels are putting you at risk for cardiovascular disease. They might suggest therapy, courses, or other initiatives that will assist you in managing your stress and minimize your chance of developing cardiac problems.
Better yet, you can strive to lessen your stress by engaging in physical activities and build a strong foundation of support by sharing or linking with supportive people and communities.